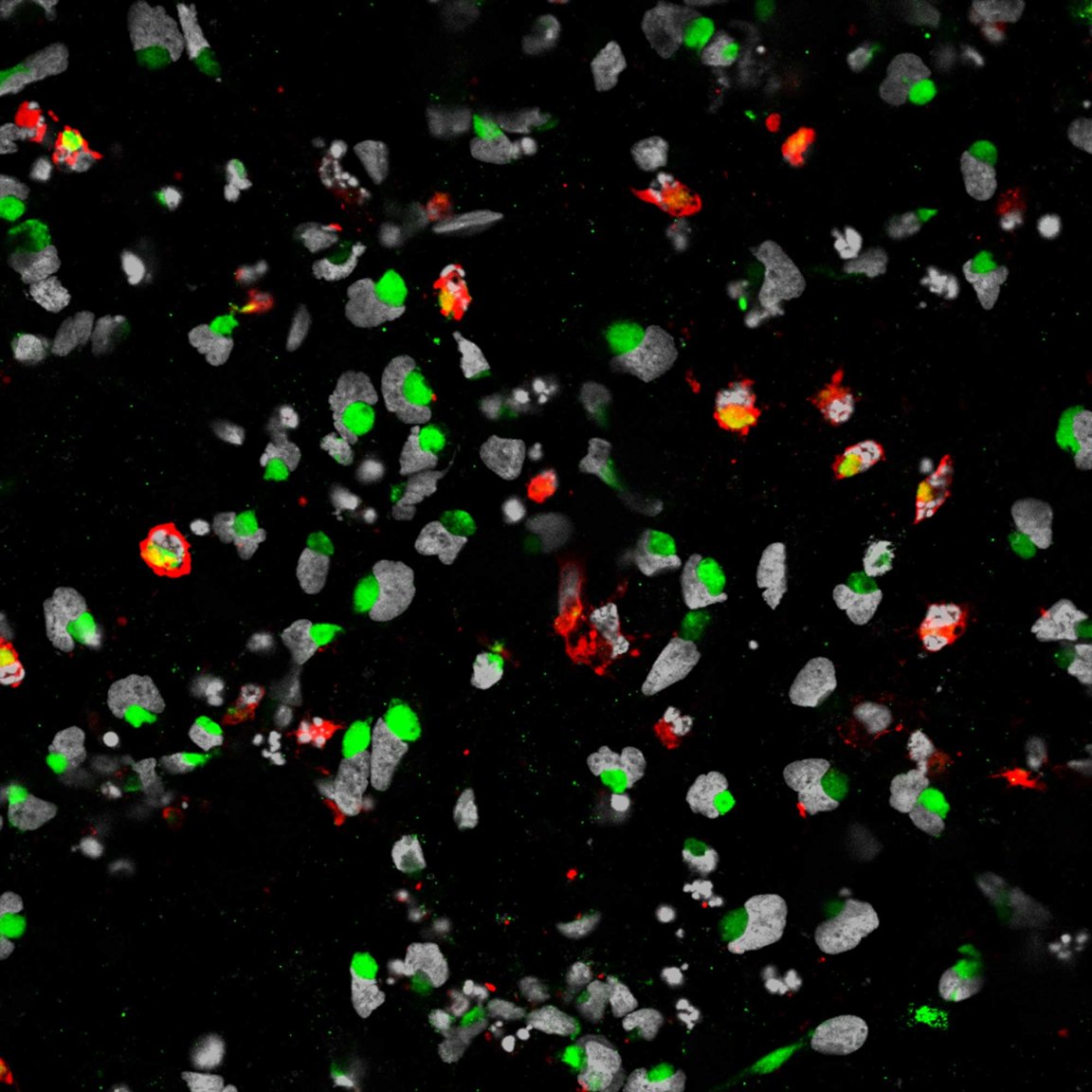
Zika kills glioblastoma cells
New research shows that although Zika virus can devastate the fetal brain, causing infants to be born with microcephaly, this same destructive power could be an effective treatment for a deadly form of brain cancer called glioblastoma. Scientists conducting the study found that the virus kills malignant brain cancer stem cells — cells which are most resistant to typical cancer treatments. If further developed and validated, this treatment could dramatically improve the outlook for patients with glioblastoma, which is usually fatal within one year of diagnosis.
Every year, approximately 12,000 people in the US are diagnosed with glioblastoma, the most common type of brain cancer. If previously unfamiliar with the illness, it might sound familiar as Senator John McCain is among those diagnosed this year. Despite the aggressive nature of the standard treatment regimen for glioblastoma, which includes surgery followed by radiation and chemotherapy, most tumors recur within six months. This is because glioblastoma stem cells often survive treatment, continuing to divide and produce new tumor cells, making glioblastoma so deadly; approximately 95 percent of patients die within five years of diagnosis, and more than half die within the first 15 months.

This research team observed that glioblastoma stem cells behaved much like neuron progenitor cells do, in that both kinds of cells are neurological and have an almost limitless ability to create new cells. Since Zika virus targets and kills neuro progenitor cells, they decided to see if it might also be able to target and kill glioblastoma stem cells. The team infected glioblastoma tumors with two different strains of the Zika virus, and found that both strains infected and killed the cancer stem cells while mostly avoiding other cells in the tumors. The researchers then injected Zika virus into brain tumors in mice to test whether the virus could treat cancer in a living animal, and found that the tumors were significantly smaller in the Zika-treated mice, who survived longer than the control group.
Complementary Treatments
These results suggest that Zika virus infection and tradition radiation and chemotherapy treatments might have complementary effects. The former targets stem cells but leaves the rest of the tumor, however, the latter kills the tumor cells and can miss the stem cells. “We see Zika one day being used in combination with current therapies to eradicate the whole tumor,” Washington University School of Medicine assistant professor of medicine and of neurology Milan G. Chheda, MD said in a press release.
It may seem scary to intentionally infect people with Zika virus; to treat tumors the virus would be injected directly into the brain, probably during surgery to remove the primary tumor and avoid triggering an immune response. However, in adults, Zika is far safer than it is in children and babies because adult brains have very few neuro progenitor cells.
The researchers have also taken steps to render the virus safer, testing it in other brain tissue and introducing mutations that weaken the virus’s ability to fight immune responses. This change makes the virus able to grow in unhealthy tumor cells, but unable to survive the robust antiviral response of healthy cells. “We’re going to introduce additional mutations to sensitize the virus even more to the innate immune response and prevent the infection from spreading,” Michael S. Diamond, MD, Ph.D., the Herbert S. Gasser Professor of Medicine at Washington University School of Medicine and the study co-senior author, said in the press release. “Once we add a few more changes, I think it’s going to be impossible for the virus to overcome them and cause disease.”