No Fear
On November 14, doctors from Toronto’s Mount Sinai Hospital and the Hospital for Sick Children confirmed via a news conference that they had successfully performed an in-utero surgery to correct myelomeningocele — a procedure that had never been undertaken in Canada before.
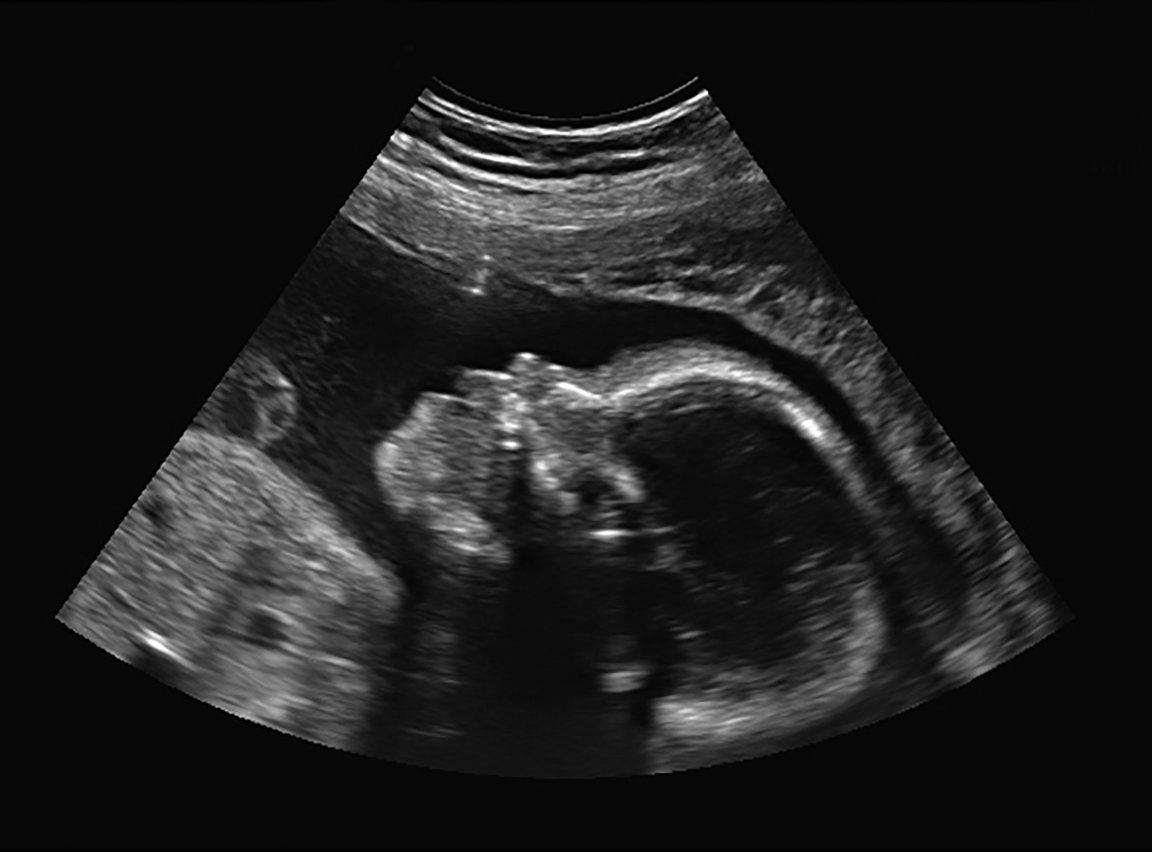
Canadian couple Romeo Crisostomo and Romeila Son learned at their 20-week ultrasound that their unborn baby had myelomeningocele, a form of spina bifida that occurs when the spinal column doesn’t close properly during the fetus’ development.
The spinal cord becomes exposed, causing damage that can lead to brain damage, various levels of paralysis, and the need for a wheelchair. Fewer than half of the children who are diagnosed with myelomeningocele are able to live on their own when they reach adulthood.
Surgeons in the U.S. had been able to successfully repair the condition in utero, so Son considered traveling south to have the surgery. However, a consultation with doctors at Mount Sinai established that it could be performed on Canadian soil.
“I wasn’t scared,” said Son, according to a report from CBC. “I had zero doubt and 100 percent confidence.”
In June, medical staff from Mount Sinai applied general anesthetic to Son and anesthetized the 25-week-old fetus using a needle inserted through the mother’s abdomen. Incisions were made into the uterus to offer access to the fetus, and the spinal defect was covered with skin. Amniotic fluid that was drained from the uterus during the procedure was replaced using a catheter, ensuring that the fetus would remain healthy during the final weeks of pregnancy.
Two months later, Eiko Crisostomo was born via caesarean section, and she is now almost three months old.
Better Care
Myelomeningocele affects between 120 and 150 children in Canada annually, and while the in-utero surgery does not guarantee that a child will not suffer from the detrimental effects of spina bifida, research shows that it significantly improves the outlook. Brain malformations are a third less likely to occur, and recipients are half as likely to require a brain shunt or the use of a walking aid or wheelchair.
“Right now, her brain is stable, her legs are moving and kicking as you can see,” said Son during the news conference. “All of our prayers were answered. She’s our little miracle.”
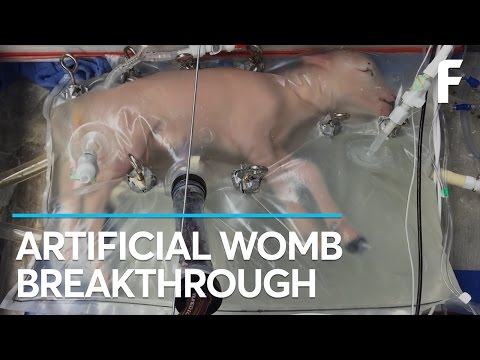
Recent advances in prenatal medicine extend far beyond the treatment of spina bifida. Clinical trials held earlier this year established that a drug first developed in the 1960s might help prevent deaths caused by blood loss during childbirth. Peptides have been successfully administered straight to the placenta, which could spell the end of premature births. There are even efforts to produce artificial wombs.
Medical advances are making pregnancy safer than ever before for mothers and babies alike. Since Eiko’s surgery in June, three other expectant mothers have visited the hospitals in Canada to have it performed, and hopefully, we’ll one day reach a point where all expectant mothers have access to the very latest in prenatal care.