Prolonged Efficacy
Without a doubt, the treatment potential of stem cell therapies is extraordinary. Yet, there is one hurdle scientists have been working to overcome: making sure the cells survive in the human body long enough to ensure they function. Well, scientists at the Buck Institute may have found a way to make it happen.
In a study published in the journal Cell Stem Cell, researchers managed to observe demonstrations of long-term vision restoration through photoreceptor transplants using human stem cells. They managed to prevent immune system rejection of the stem cells, blocking the usual immune responses that trigger rejection of the stem cells by the recipient’s body.
Originally, it wasn’t clear whether the transplanted photoreceptors simply died out before being effective or if they were shut down by the body’s immune system. Lamba explained that scientists thought the eye and the brain were exempted from monitoring by the immune system’s cells. To figure it out, the team studied a specific mouse strain that was healthy, but lacked a particular immune cell receptor called IL2rγ. These immunodeficient IL2 receptor gamma (IL2ry) null mice are unable to reject transplanted foreign cells.
These mice showed a ten-fold increase of living human embryonic stem cell-derived donor retinal cells. The transplanted retinal cells matured and successfully integrated into the mice’s retinas.
“This turned into a nice story of long-term restoration of vision in completely blind mice,” said Deepak Lamba, senior author. “We show that these mice can now perceive light as far out as 9-months following injection of these cells.”
It’s Not the Immune System, Is It?
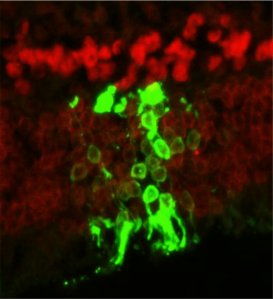
Seeing how the transplants were able to survive, the researchers needed to test if they actually worked. Stem cell-derived photoreceptors were inserted into a strain of congenitally blind mice. By measuring their pupils’ response to light and their brains’ visual response centers (to check if signals from the eye were reaching the appropriate brain areas), the researchers observed that the mice were able to see again.
“That finding gives us a lot of hope for patients, that we can create some sort of advantage for these stem cell therapies so it won’t be just a transient response when these cells are put in, but a sustained vision for a long time,” said Lamba. “Even though the retina is often considered to be ‘immune privileged,’ we have found that we can’t ignore cell rejection when trying to transplant stem cells into the eye.”
To further improve the process, the team is already studying the use of approved drugs that target inhibiting the IL2ry receptors to prevent transplant rejection in the eyes. “We can also potentially identify other small molecules or recombinant proteins to reduce this interleukin 2 receptor gamma activity in the body – even eye-specific immune responses – that might reduce cell rejection,” Lamba explained. “Of course it is not validated yet, but now that we have a target, that is the future of how we can apply this work to humans.”