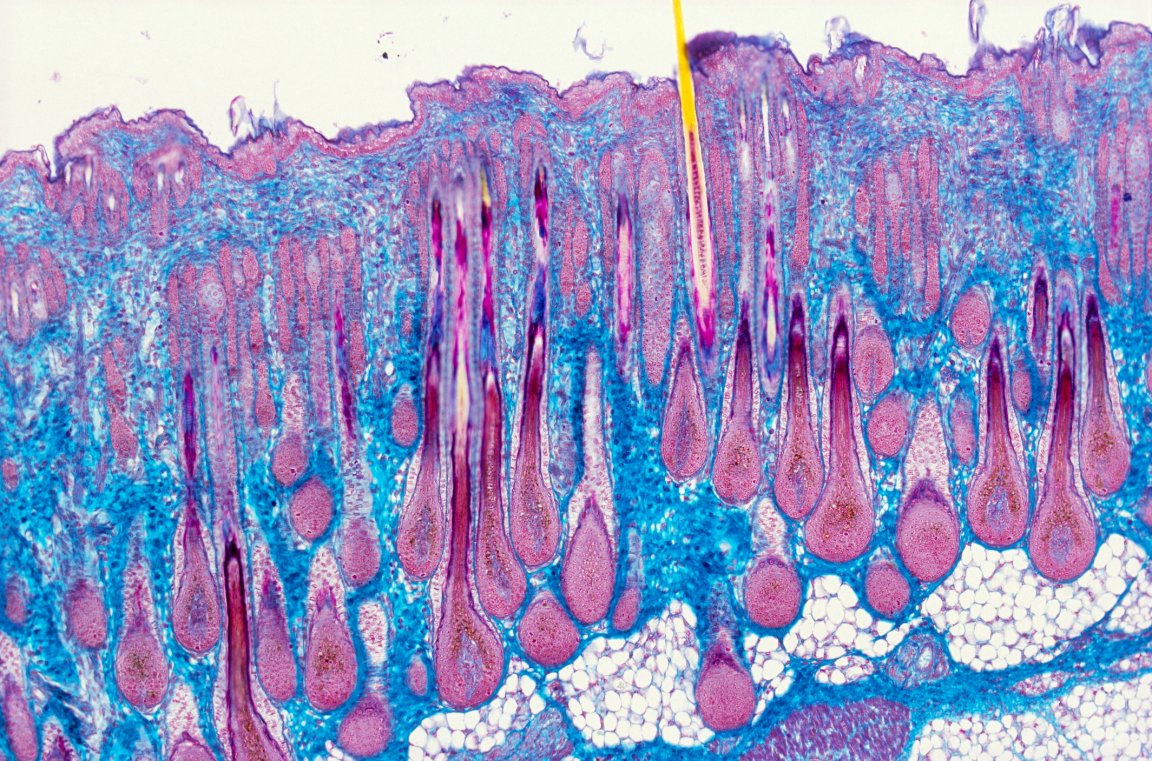
Cellular Renovation
Why build something from the ground up when one can just renovate an already existing structure? Essentially, that’s what researchers from the University of Washington School of Medicine in St. Louis had in mind when they developed a method for transforming adult human skin cells into motor neurons in a lab. They published their work in the journal Cell Stem Cell.
“In this study, we only used skin cells from healthy adults ranging in age from early 20s to late 60s,” senior author Andrew S. Yoo said in a press release. “Our research revealed how small RNA molecules can work with other cell signals called transcription factors to generate specific types of neurons, in this case motor neurons. In the future, we would like to study skin cells from patients with disorders of motor neurons. Our conversion process should model late-onset aspects of the disease using neurons derived from patients with the condition.”
They did this by exposing skin cells in a lab to certain molecular signals usually found at high levels in the human brain. They focused on two short snippets of RNA: microRNAs (mRNAs) called miR-9 and miR-124, which are involved in repurposing the genetic instructions of the cell. These mRNAs, combined with certain transcription factors, successfully turned skin cells into spinal cord motor neurons within just 30 days. These new cells closely resembled normal mouse motor neurons in terms of which genes were turned on and off, and how they functioned.
Better Understanding and Improved Treatment
Usually, when researchers find ways to replace damaged cells or organs, they resort to using stem cells. In particular, they use embryonic stem cells (a type of pluripotent stem cells) to grow the cells or organs needed.
While this type of stem cell has the potential to grow into whatever adult cell type is needed, the procedure carries some ethical concerns. In bypassing a stem cell phase, the new cell transformation technique doesn’t have any of these ethical issues.
Keeping the original age of the converted cells can be crucial for studying neurodegenerative diseases that lead to paralysis, such as amyotrophic lateral sclerosis (ALS) and spinal muscular atrophy, the condition the new research focused on. In particular, researchers hope that it could enhance the understanding of these diseases in order to improve regenerative medicine.
“Going back through a pluripotent stem cell phase is a bit like demolishing a house and building a new one from the ground up,” Yoo explained. “What we’re doing is more like renovation. We change the interior but leave the original structure, which retains the characteristics of the aging adult neurons that we want to study.”
Like embryonic stem cells, the technique can also allow for converting human skin cells into other cell types by using different transcription factors. Before this technique can be applied to actual humans with neurodegenerative diseases, the researchers still need to find out how much the cells made in their lab match native human motor neurons. Still, it’s a promising start.