A New Treatment for Macular Degeneration
Macular degeneration is the leading cause of progressive vision loss with almost 10 million Americans affected by the disease. Currently, there are no known cures for the condition — although stem cells might change that entirely.
Macular degeneration occurs when the central portion, the macula, of the retina is deteriorated. This is where our eyes record images and send them to the brain through the optic nerve. The macula is known for focusing our vision, controlling our ability to read, recognize faces, and see objects clearly.
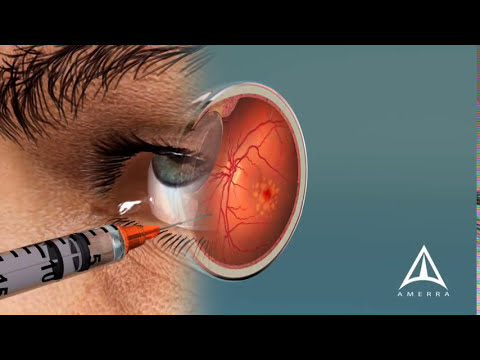
A Japanese man in his sixties is the world’s first person to receive induced pluripotent stem (iPS) cells donated by a different individual. Rather than tip-toeing around the ethics of embryonic stem cells, scientists were able to remove mature cells from a donor and reprogram them into an embryonic state, which then could be developed into a specific cell-type to treat the disease. Physicians cultivated donated skin cells that were transplanted onto the man’s retina to halt the progression of his age-related macular degeneration.
While the man’s first surgery was a success, the doctors have said they will make no more announcements about his progress until they have completed all five of the planned procedures. While the effectiveness of this technique cannot be evaluated until the fate of the donated cells and the progression of the patient’s macular degeneration have been fully monitored, there is increasing interest in using iPS cells for theraputic purposes.
Sharing Stem Cells
A similar therapy was performed at the Kobe City Medical Center General Hospital in Japan in September 2014, but with a slight difference. In this case, the patient received her own skin cells reprogrammed into retinal cells. As hoped, a year after the surgery her vision had no decline, seemingly halting the macular degeneration. Four more patients in the clinical trial are expected to receive donor cells as well.
The donor-cell procedure, if successful, could help pave the way for the iPS cell bank that Shinya Yamanaka is establishing. An iPS cell bank would allow physicians find the perfect iPS donor per each patient’s biological signatures. Yamanaka is a Nobel-prizewinning scientist at Kyoto University who pioneered the iPS cells.

Yamanaka’s idea of a iPS cell bank has the potential to revolutionize modern medicine. It would provide patients with ready-made cells immediately, giving a widespread population access to more treatment options by lower all-around costs. While the risk of genetic defects or a poor donor match still remains, the new procedure could offer enormous advantages compared to other alternatives.