Before we get to the therapeutic stuff, here is a reminder of the main problem people with Parkinson’s disease face.

Researchers are reasonably sure that the accumulation of a protein called alpha-synuclein is responsible for neurons dying in people with PD. However, there are two competing theories as to how it builds up and spreads, the threshold theory and the ascending theory (also called the prion hypothesis). The ascending theory states that alpha-synuclein spreads from cell to cell, ‘infecting’ cells as the protein moves up through the brain. The threshold theory recently put forward by Dr. Ole Isacson and Dr. Simone Engelender, proposes that alpha-synuclein builds up independently in each affected cell.
Regardless, an improved understanding of exactly how such proteins misfold and clump together is at the heart of the riddle that is Parkinson’s as well as a long list of other diseases. Thankfully a number of labs around the world have been working on this sticky problem. Additionally, if anyone wants to help you can do so very easily from any computer, watch this video to learn how.

The Age of Personalized Medicine
The ongoing revolution in genetics is playing an increasingly important role in our understanding of the disease while also revealing why it varies so much from patient to patient. There have been dozens of mutations and variants associated so far with the disease. We are just beginning to understand the role our genes play in the development of neurological diseases but an immense amount of progress has been made in the last 15 years since the human genome was sequenced. Now that sequencing costs have plummeted to around a thousand dollars we are on the verge of a new era in medicine that promises to give patients treatments tailored to their specific condition.
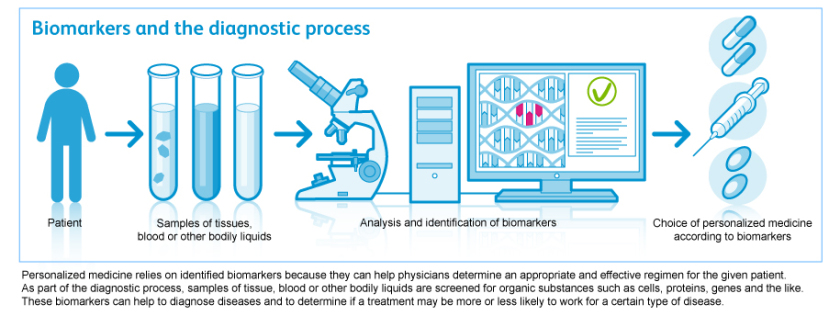
“Personalized medicine is healthcare based on your unique genetic and molecular blueprint. Each individual has distinct genetic makeup, biomolecule and metabolic profiles, set of gut microbes, and so on. Similarly, there is no one-size-fit-all in healthcare. How you stay healthy or how you are treated for disease should be catered to match your unique profile. Knowledge of your genomics, proteomics, metabolomics, microbiotics, and other bioinformatics allow for the improvement in the quality of life, from disease prevention to therapy best suited to you.” (from the Personalized Medicine Initiative in British Columbia.)
A better understanding of genetics will help unlock a cascade of other problems that surround this disease including mitochondrial dysfunction, lysosomal degradation, neuroinflammation, gut bacteria, and epigenetics, among others. And thankfully there is now a large interconnected global community of researchers working to solve these problems with more resources and better tools than in all of human history combined. This growth in a variety of public and private sector health initiatives across disciplines has lead a growing number of experts to believe that we will make more progress in the next decade than we did in the past century, which is good reason to be hopeful considering what medicine was like a hundred years ago.
This medical revolution will be further bolstered by new and improved imaging techniques. A big part of the problem we still have with this disease is that we can’t actually see what is wrong. Every person who has PD has slightly different symptoms but we don’t really know why primarily because we can’t accurately see inside patient’s heads. Soon a new line of imaging techniques will be available that will give surgeons and researchers a much better understanding of what is going on inside the heads of each patient.
In addition, there are some immense ongoing collaborations such as the European human brain project and the U.S. brain initiative that are trying to do for the brain what the human genome project did for our understanding of the genome. If successful it will give researchers unprecedented insight into how our minds are pieced together.
Then there are the new therapies themselves.
Current Treatments That are Getting Better Every Day
Levadopa – For 50 years now this wonder drug has brought relief to millions. Of course, problems still persist, namely in getting it past that stubborn blood brain barrier and making sure a more steady supply is delivered to reduce on/off fluctuations. To get around some of those problems we now have patches, slow release and extended release capsules, as well as intestinal pumps that deliver a steady flow of the drug directly into the intestines. Of course this drug is not an ideal solution as there are nasty side effects that come from long term use, predominantly dyskenisia which gives people the motor control of a blob of jelly, but for now, it is still the best stop-gap solution we have.
Deep Brain Stimulation – This science-fiction wonder has become the undisputed Queen of modern treatments. It has already proven itself to be a miracle worker, re-animating hundreds of thousands with its electric wizardry. It too is steadily improving, from John Palferman’s book, Brain Storms, “Instead of implanting devices that simply deliver a continuous electrical stimulation, they are developing technologies that deliver stimulating jolts only when required. ..The idea is to design DBS so that the system can monitor the electrical activity in the basal ganglia, and when it detects an abnormal signal, it can respond automatically with an appropriate stimulation. A smart device…”
Therapies Soon to be Available (2 to 5 Years)
New Drugs – There is a long list of promising drugs that are already in clinical trial. Some of these drugs have the potential to not only offer symptomatic relief but hit the holy grail that is actual disease modifying therapies.
Neuromodulation techniques – A number of novel neuromodulation techniques are being tested for clinical use. The most prevalent is called transcranial magnetic stimulation in which magnets are attached to the outside of patient’s heads that send a focused electric current deep into the target areas of the brain. Already an approved therapy for depression, TMS is now being tried in PD.
Therapies on the Horizon (5 to 10 years)
Immunotherapies – The relatively recent identification of alpha-synuclein as playing a key role in disease formation has lead researchers to believe that we may be able to harness the bodies immune system to stop the protein from clumping while also mitigating the bodies natural inflammatory responses that damages neurons.
Pharmacogenetics – The genetic revolution has spurred the development of a relatively new field of pharmacology called pharmacogenetics. Eventually, instead of making one drug for everybody, we will be able to tailor drugs to better fit each person’s unique condition.
Stem Cell Therapies – Though there were a series of trials in the 90’s that had mixed results, recently a number of labs around the world have begun reexamining the therapeutic potential of stem cells. This is thanks in part to the 2007 discovery of a new type of stem cell called IPS cells which allow researchers to grow fully functioning stem cells from patient’s own skin cells. This has opened the door to a new set of therapies while also giving us better disease models. Since those first trials we have also made a series of other advances in our understanding of how to use stem cells which has lead to some stunning results in trials on other apes. Some labs are hoping to push forward with human trials starting at the end of this year.
Gene Modification Therapies – As discussed earlier, the field of genetics is blowing up and one of the biggest benefits to society that will come from it is a new set of therapies called gene modification therapies. The most popular one today is called CRISPR, a technique that already allows researchers to cut and paste genetic code, changing the genome of living organisms. A number of articles have come out touting these kind of gene-editing techniques as the future of medicine. This first use of CRISPR was in a lung cancer patient in China last fall, but it is also being used to help us understand neurodegenerative disorders including Parkinson’s disease.
Future Treatments (10+ years)
Direct Programming – In conjunction with gene therapy, direct programming is believed to be the final solution to the problem of neurodegeneration. It is a subset of the new field of synthetic biology that will eventually allow us to change cell types in living organisms. For example, in people with Parkinson’s disease we will be able to reprogram other healthy cells in the affected area, such as glial cells or astrocytes, and directly turn them into dopamine-producing cells.
And If All Else Fails, Perhaps Robots Will Figure It Out
When it comes right down to it, the reason why we have not been able to cure a lot of the diseases that are still with us today, such as neurodegeneration or cancer, is that there are an incredible number of factors to consider when trying to treat them, possibly too many for any human, or even any group of humans, to make sense of. But there might be a solution to this problem as we are now figuring out ways to export more and more of our intellectual abilities into computers. Already computers have become as good as humans at diagnosing certain conditions, and a staggering number of healthcare companies have now invested heavily in applying artificial intelligence to the medical industry. This, along with further advances in nanotechnology, has a lot of potential in helping us understand diseases such as Parkinson’s and may reveal novel insights into how to treat them.
